Story by Ebony Ford
Most kids dream of being a doctor, astronaut, veterinarian or some other profitable occupation. Although I had similar career aspirations, I knew at an early age that I wanted to be a wife and a mother.
And in 2012 the first of those dreams came true—I married my best friend. From there I thought that if my husband just looked at me the right way that I would get pregnant. I couldn’t have been more wrong. The next 6 years were filled with loss, unexplained infertility and heart-wrenching disappointment. One doctors words to my husband & I still hurt to recount. While walking in the room she looked down at my chart and said “You know, sometimes you just have to be honest and stop kidding yourself. You have to know when to quit.” Those words not only pierced my heart like a knife but they also hacked at my hope like a machete for the next 3 years.
By the fall of 2017 I had focused my energy in other areas like earning a Bachelor’s degree. But there was always a hole in my heart where I knew a child should be. During the first week of October I began to experience what I knew to be pregnancy symptoms but amplified. As the days went by the fear of disappointment just wouldn’t allow me to open my heart or mind. After a week of my husband practically BEGGING me, I finally gave in and took a pregnancy test. Before I could sit it down on the counter, I saw the test line turn and I screamed!! WE WERE FINALLY PREGNANT! From that moment on my pregnancy was an absolute DREAM. I was followed by a high-risk fetal medicine doctor, seen twice a month, had lab work and ultrasounds performed at every appointment.
At my 24-week appointment, I learned that my doctor had an emergency and I’d be seeing one of her partners. During the visit, I was seeking clearance to fly cross-country with my husband for a show and our babymoon. I did have a bit of swelling in my ankles but the doctor wasn’t at all concerned because my blood pressure was great. He also said that I didn’t need to do repeat lab work.
I felt great on our first day in Las Vegas but just wanted to rest before our schedule picked up the next day. By morning I noticed hand and feet swelling and at the end of that night my legs were so swollen that I could barely walk. I remember thinking “What if I got a blood clot in my lung from the flight?” But I quickly dismissed that theory because I didn’t have shortness of breath. I put my feet up in between the various events that we were a part of. That evening I became winded while walking and overnight I couldn’t lay flat to sleep. I decided to send my doctor a message with a timeline of symptoms as well as my concern about going to the ER while in Las Vegas. Meanwhile, I was sitting straight up in bed on Web MD trying to self-diagnose AND convince myself that I was ok. Oxymoronic right? She advised that I return home immediately and we did.
We made it to the airport but it became harder to walk and breathe so we flagged down an airport employee who wheeled me through security and to our flight. Towards the middle of our flight I began experiencing a nagging pain in my upper abdomen. I went to reach for my purse and realized that my feet were bursting the seams in my shoes. I took two Tylenol to help the pain in my stomach and then realized that not only had I not been to the bathroom (despite drinking all flight), but I also hadn’t eaten in over 20 hours. Upon landing my vision took a turn for the worst and I lost the ability to see color. We dropped our luggage off at home and then headed to the hospital.
I was wheeled up to Labor & Delivery where after sharing my symptoms a nurse told me “Oh I’m sure you’re fine love. But since you’re not in labor and your concerns aren’t ‘pregnancy related’, you’ll need to be seen in the Emergency Room.” She then took the blood pressure cuff off of my arm stating that it wouldn’t read. I waited close to 10 min before someone wheeled me down to the ER and shared my symptoms. The triage nurse took my vitals and as soon as the numbers came up her eyes lit up as she stopped talking and turned to hit a red button on the wall. Seconds later what seemed like a dozen people came running and helped lift me out of the wheelchair onto a stretcher. As they rush me down the hallway, I heard someone say “Call a brain attack! BP 262/148”
The next hour was filled with lab work, x-rays, fetal monitoring as well as trying different medicines to lower my blood pressure. Finally, a doctor came in and said “Mrs Ford, I’m afraid you have preeclampsia. Your blood pressure has barely been touched by these medications and you have quite a bit of protein in your urine. I’m waiting for a few more tests but I can assure you that you won’t be going home today. I can only keep you pregnant until 32 weeks with preeclampsia. So, you’ll be staying here on the L&D unit until you deliver.” Although I wasn’t happy about the diagnosis or having to remain inpatient, I was relieved that my baby was fine and that I now knew what was wrong.
And before my husband & I could even accept or share that news, 3 doctors came to the foot of the bed with facial expressions I’ll NEVER forget. They told us that not only did I have sudden onset SEVERE preeclampsia but I also had something called HELLP syndrome, was in kidney and liver failure and needed to deliver my daughter IMMEDIATELY via emergent cesarean section. I would also likely spend the next few days in the ICU recovering due to the multi-organ failure. It was as if time stood still and the weight of their words hit me like an 18-wheeler. I was going to deliver my baby at just 26 weeks!! What would a 26-week-old baby look like? How much would she weigh? WOULD SHE SURVIVE? These were all the questions that flooded my mind as they rushed me up to L&D and removed my remaining clothing.
My husband began notifying close family & friends. As I listened to him breaking the news over and over a doctor introduced herself as a NICU doctor and began sharing words that haunted me for months to come—“Mrs Ford you should know that although your baby is viable, she’s susceptible to respiratory failure and may not be able to breathe on her own. There could be issues getting the breathing tube in causing permanent esophageal, trachea and vocal cord damage. She could have brain bleeds requiring brain surgery, seizures and has a very high chance of having cerebral palsy, developmental delays and other complications. We need you to know all of these things so that you know what to expect for the next few months that you’ll be in the NICU with your baby.” Next few MONTHS?! Cerebral palsy? Brain bleeds? Brain SURGERY? Another doctor came in and told me that I would be delivering my baby under general anesthesia so that I could be sedated and intubated to relieve my lungs from the pulmonary edema caused by preeclampsia.
But the most crushing part was that my husband wouldn’t be able to be in the OR along with the surgical, NICU and ICU teams who were ready to care for us both. I said goodbye to my husband and family for what felt like the very last time. As I was wheeled to the OR fear enveloped me and all I could think was “This is it! I’m not gonna make it. He’s going to raise our baby alone. Why me? Why now? Why US?” As they transferred me to the operating table a nurse held my hand and whispered a prayer in my ear. That’s the last thing I remember before falling asleep.
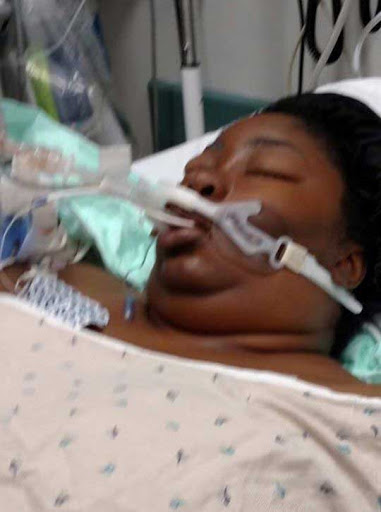
When I opened my eyes again, I was alone in a very large and empty room. Although very groggy I could see that the clock on the wall said 12:15 pm. I felt an uncomfortable pressure in my chest and realized that I was still on a ventilator. I tried to lift my hands and feet but couldn’t as I was tied to the bed. I began to panic and cried for what felt like an eternity before 2 doctors came in the room and explained that my c-section went well but that the birth didn’t immediately resolve the preeclampsia, HELLP Syndrome or multiorgan failure but I was able to avoid needing a liver transplant. The ventilator was then stopped and the breathing tube removed.
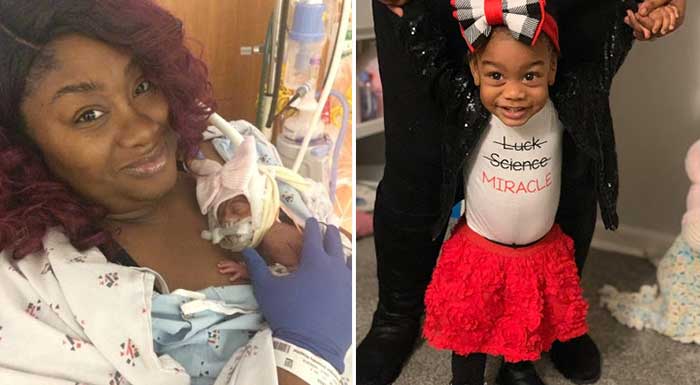
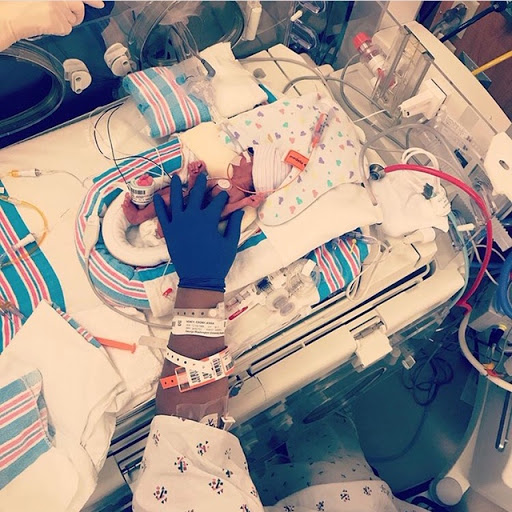
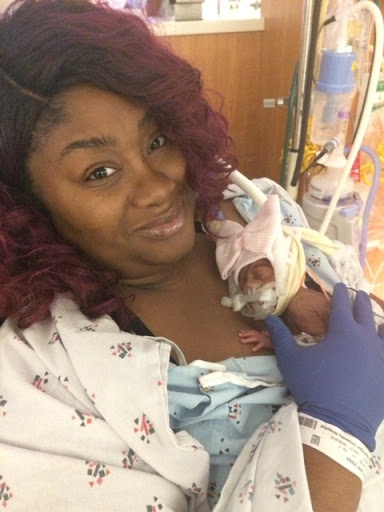
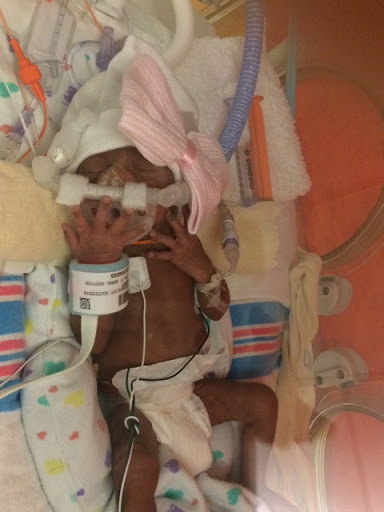
My husband came in the room shortly after that and told me that our daughter was born at 6:32 pm, weighed 1lb 15oz, is 15.5 inches (VERY long for a 26 weeker) and was doing great! About 12 hours later my blood pressure and liver enzyme count improved enough to be moved to Labor & Delivery. I was so drugged, sedated and groggy but I couldn’t rest until I laid eyes on my little miracle. They wheeled me to her incubator and as they lowered her bed I laid eyes on the tiniest baby I had ever laid eyes on. She was kicking, flailing her arms and being the sassy fighter we would come to know her as. I touched her finger and she grabbed my finger with all her might. It was then that I knew not only would she but WE would be just fine.
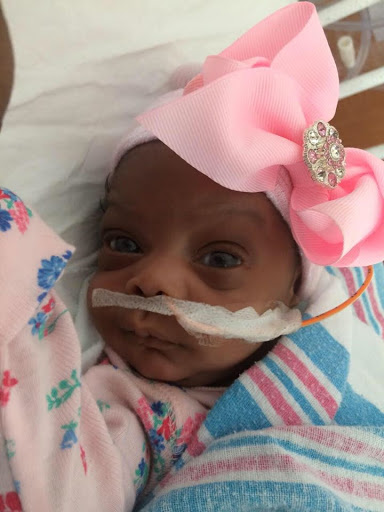
I learned that she did come out breathing on her own but they put her on a ventilator as a preventative measure. But our little fighter insisted on breathing at her own pace causing her right lung to tire and collapse. It then happened a few days later on the other side. So, by her 5th day of life, Reign had experienced 2 lung collapses, chest tubes and blood transfusions. She then somehow got the strength to pull out her breathing tube and was breathing on her own for close to a minute before anyone discovered what she had done. They decided to leave the tube out and put her on bubble CPAP, a form of nasal oxygen that helps develop the lungs as well. She did great with that and by week 7 she grew tired of that too and pulled it off as I watched on camera from home to see if anyone would run to put it back on. Turns out that her vitals never changed proving that she could breathe WITHOUT help. The oxygen never went back on.
And for the remainder of her time in the NICU, Reign led the way on her milestones. She had a total of 8 blood transfusions and needed phototherapy for jaundice twice but overall had an amazingly uneventful 80-day journey in the NICU. She left the NICU weighing 6lb 10oz 3 weeks before her doctor’s predictions without oxygen, monitors, medications or any of the other standard care items that most micro preemies come home with. Her homecoming was quite a celebration for not only our family but also the social media followers all around the world who had grown to love her, pray for her and keep up with her progress via social media, family and friends sharing this miracle of hope with them.
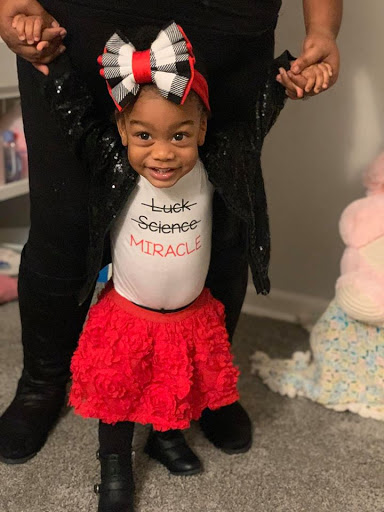
Although she came home completely healthy, her lungs proved to still be extremely premature and no match for the fall/winter of 2018. She contracted croup, bronchiolitis, pneumonia and RSV twice, the second bout being far more deadly. As a result of the damage done to her lungs, she became oxygen dependent in the spring of 2019. Despite those initially grim predictions for development, Reign still met all of her milestones within normal range and weighs a healthy 25 lbs. Because of our journey with prematurity, a near death birth story and parenting a medically fragile child, we decided to turn our pain into advocacy by becoming ambassadors for March of Dimes as well as mentoring other NICU, preemie and medically fragile parents through our Instagram profile and our Website. We were most recently a part of March of Dimes “It’s Not Fine” campaign commercial and print ads. We hope that through sharing our story so openly that no other parent feels as alone as we once did and knows that despite the circumstances presented, they too can REIGN!
You can follow their journey on: Instagram and Website